If you’ve been researching therapy options, you’ve probably come across two approaches more than any others: EMDR and CBT. Both are well-researched, widely recommended, and used every day to help people work through trauma, anxiety, and some of life’s heaviest experiences.
So which one is right for you?
It’s a question worth taking seriously, and one that doesn’t have a single answer. The comparison of EMDR vs CBT isn’t really about which therapy is superior. It’s about which approach fits where you are right now, what you’re carrying, and how you want to heal.
This guide walks you through both therapies honestly. What they are, how they work, what the research shows, and how to find your footing when choosing between them.
What Is EMDR Therapy?
EMDR stands for Eye Movement Desensitization and Reprocessing. It was developed in the late 1980s by psychologist Francine Shapiro, originally to help people process traumatic memories that had become stuck: vivid, emotionally loaded, and easily triggered.
How EMDR Works
The premise is rooted in how the brain stores memory. When something overwhelming happens, the brain can struggle to fully process that experience. Instead of integrating it like an ordinary memory, it gets frozen. It often surfaces as flashbacks, physical tension, or emotional reactivity that feels disconnected from the present.
EMDR works by gently activating that memory while simultaneously engaging the brain’s natural processing system through bilateral stimulation, typically guided eye movements, alternating taps, or sounds. Over time, this process helps the memory lose its emotional charge, changing your relationship to it. It won’t erase what happened or make the memory disappear, but it can help you connect with it in a new way.
EMDR is structured across eight phases, from history-taking and stabilization through active reprocessing and integration. You don’t have to recount the traumatic event in detail to move through it, which many clients find to be a significant relief.

What EMDR Is Used For
EMDR therapy is most commonly used for:
- Trauma and PTSD
- Grief and loss
- Performance anxiety
- Low self-worth
- Feeling emotionally “stuck” even after years of talk therapy
This EMDRIA article also outlines some of the other challenges EMDR has been known to treat in adults and children.
What Is Cognitive Behavioral Therapy (CBT)?
CBT, or Cognitive Behavioral Therapy, is one of the most widely practiced therapeutic approaches in the world. Developed in the 1960s by psychiatrist Aaron Beck, it’s built on a foundational idea: how we think affects how we feel, and how we feel affects how we behave.
How CBT Works
CBT is structured and goal-oriented. Therapist and client work together to identify patterns of unhelpful thinking — called cognitive distortions — and the behaviors that follow from them. From there, you develop practical tools to challenge those patterns and build new responses.
Sessions tend to feel conversational and skills-focused. You’ll often leave with something concrete to practice between appointments such as journaling, thought records, or behavioral experiments. Progress is tangible, which many clients find grounding.how
To learn more information about how it works, check out this Psychology Today article.
What CBT Is Used For
CBT is one of the most versatile therapies available. It’s commonly used for:
- Anxiety and panic
- Depression
- OCD
- Eating disorders
- PTSD
- ADHD
- Life transitions and chronic stress
EMDR vs CBT: Key Differences
While both are evidence-based and effective, EMDR and CBT operate quite differently in practice. A few of the most meaningful distinctions:
Focus: CBT works in the present by identifying and restructuring unhelpful thoughts and behaviors. EMDR works with the past by reprocessing specific memories or experiences that continue to drive present-day distress.
Approach: CBT is largely cognitive and behavioral, working through analysis, conversation, and skill-building. EMDR is more somatic and memory-based, engaging the brain’s own processing system through bilateral stimulation.
Session experience: CBT often feels like a structured conversation. EMDR sessions can feel more internal, which may cause clients to notice strong emotions or body sensations during processing, followed by a noticeable sense of release.
Homework: CBT frequently involves between-session practice. EMDR is more contained within sessions, though grounding and stabilization tools carry over into daily life.
Talking about trauma: CBT-based trauma approaches like Cognitive Processing Therapy (CPT) do involve revisiting traumatic content. In EMDR vs CBT for trauma, a key difference is that EMDR allows processing without requiring detailed verbal retelling, which can feel like a meaningful distinction for those who find recounting events retraumatizing.
Here’s a side-by-side view:
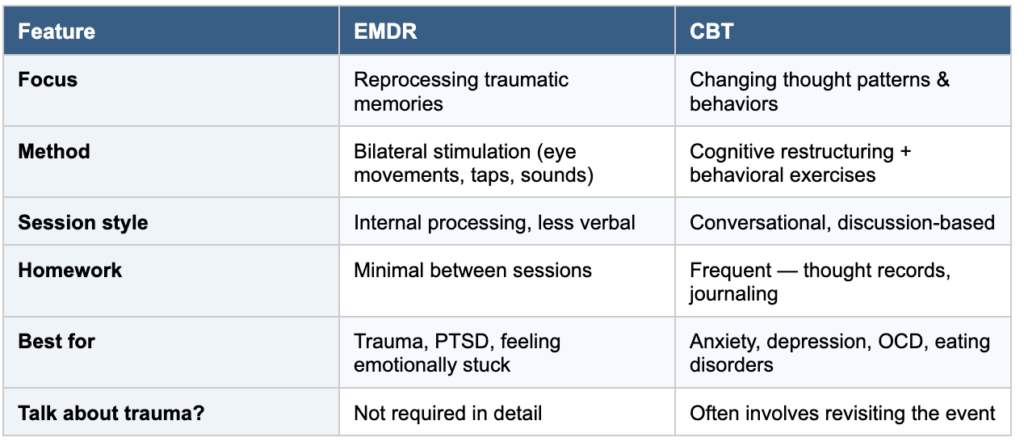
Curious if either one is a right fit?
Schedule a complimentary consultation with our trained professional, Dylan Beckner, to help you decide which is the best approach for you. Each case is unique, and approaches can vary depending on several factors. Answering the EMDR vs CBT dilemma can be quite difficult, so do not hesitate to get professional advice before deciding.
EMDR vs CBT for Trauma and PTSD
This is where the comparison is most clinically significant and where the research is most robust.
Both EMDR and trauma-focused CBT are recognized as first-line treatments for PTSD by the American Psychological Association and the World Health Organization. Multiple meta-analyses have found them similarly effective at reducing trauma symptoms overall. That’s important to name: neither therapy has a decisive advantage in the research.
That said, some studies suggest EMDR may produce faster symptom reduction in certain populations — particularly when trauma has a clear, identifiable origin. Other research finds CBT-based approaches like CPT and Prolonged Exposure equally strong, especially when cognitive distortions (shame, self-blame, distorted beliefs about safety) are driving the distress.
In practice, many clients respond more strongly to one approach than the other. That’s less about data and more about fit: how the therapy feels in the room, what it asks of you, and what you’re ready for.
You might lean toward EMDR if: you feel like you’ve processed the trauma cognitively but the emotional weight is still there, or if talking about what happened in detail feels too overwhelming.
You might lean toward CBT if: you want a structured, skill-building approach, or your distress is driven by specific thought patterns you want to actively challenge.

Which Therapy Works Better?
Research consistently shows both therapies are highly effective. The best choice between EMDR vs CBT depends on your symptoms, your goals, and how you prefer to engage in therapy.
What the research does suggest is that certain factors predict outcomes more reliably than which specific modality you choose:
- A strong, trusting relationship with your therapist
- A clear understanding of what you’re working on and why
- Showing up consistently and engaging honestly in the process
- Feeling safe enough to be present in sessions
These conditions matter more than technique alone. While modality does play a role, it’s not the most critical factor. When someone asks whether EMDR or CBT works better, the most accurate answer is: the one that fits you best and is delivered by a therapist you trust.
Benefits of EMDR Therapy
- Can produce meaningful results in fewer sessions than traditional talk therapy
- Processes trauma without requiring detailed verbal retelling
- Addresses how trauma is held in the body, not just the mind
- Effective for complex trauma, single-incident trauma, grief, and anxiety
- Recognized by the APA, WHO, and VA as a first-line treatment for PTSD
For more on what EMDR therapy looks like at our Leesburg practice, visit our EMDR therapy page.
Benefits of Cognitive Behavioral Therapy
- One of the most extensively researched approaches in psychotherapy
- Builds lasting, practical skills that extend beyond the therapy room
- Highly adaptable across anxiety, depression, OCD, eating disorders, ADHD, and more
- Structured format works well for people who appreciate measurable progress
- Foundational to many other evidence-based approaches including DBT, ACT, and ERP
How to Choose Between EMDR and CBT
Take the Next Step
That’s what the intake process is for. You don’t have to figure this out by tossing coins or desperately scrolling on the internet.
When you connect with a therapist at Beckner Counseling, you’ll start with a complimentary consultation to talk through what’s bringing you in, what you’ve already tried, and what you’re hoping for. From there, your therapist will recommend an approach or a combination of approaches based on your needs.
As a starting point:
Signs EMDR Might Be a Good Fit
- You understand your trauma intellectually but still feel it in your body
- Talking through what happened in detail feels retraumatizing
- You’ve done talk therapy before and feel emotionally stuck
- Your distress is tied to a specific event or period in your life
Signs CBT Might Be a Good Fit
- You want a structured, skill-building approach with clear steps
- Your distress is shaped by thought patterns you want to actively challenge
- You’re working through anxiety, OCD, or depression alongside trauma
- You prefer a more conversational therapy format
Many people end up using both. CBT as a foundation for building skills and emotional regulation, and EMDR to process specific memories that continue to surface. In that way, the EMDR vs CBT question becomes less of a choice and more a plan as to when the right time is to introduce each.
The question isn’t really which therapy is better. It’s which therapy is better for you, right now, with the right therapist beside you.
EMDR and CBT are both powerful tools. They work differently, they feel different in the room, and they suit different people at different points in their healing. Knowing the difference between them is a meaningful first step. Reaching out to talk it through is the next one.
You don’t have to have it figured out before you call. We’ll figure it out together.
Frequently Asked Questions
Is EMDR better than CBT?
Research doesn’t consistently crown one as superior. Both are highly effective, particularly for trauma and PTSD. EMDR may work more quickly for some clients; CBT offers broader versatility across conditions. The best choice depends on your specific needs, history, and what you’re hoping to accomplish in therapy.
Can EMDR replace CBT?
For some clients and some goals, yes. For others, no. Many therapists use both in combination — particularly when a client is working on both trauma processing and behavioral change. It’s rarely a strict either/or situation in practice.
Which therapy is better for trauma?
Both EMDR and trauma-focused CBT are first-line treatments for trauma and PTSD, recognized by the APA and WHO. Some meta-analyses show EMDR with a slight edge in symptom reduction speed; others find comparable outcomes. A trauma-informed therapist can help you assess which approach fits how your trauma is presenting.
How long does EMDR therapy take?
For a single-incident trauma, many clients see meaningful progress in 6 to 12 sessions. Complex or developmental trauma often takes longer. Your therapist will give you a clearer picture after your intake session.
Is CBT effective for PTSD?
Yes. Trauma-focused CBT approaches like Cognitive Processing Therapy (CPT) and Prolonged Exposure (PE) have strong evidence bases for PTSD. They’re particularly effective when cognitive distortions — shame, self-blame, distorted beliefs about safety — are a significant part of the picture.







